TOPICS
Showing posts with label HRCT. Show all posts
Showing posts with label HRCT. Show all posts
Sarcoidosis- CT findings
By Dr Deepu
 |
| conglomerated micronodules and centrilobular nodules in both lungs |
 |
| Enlarged mediastinal lymph nodes |
 |
| Bilateral hilar lymph nodes |
Chest CT scans show conglomerated micronodules
and centrilobular nodules in both lungs. We can see the enlarged mediastinal
and bilateral hilar lymph nodes.
Sarcoidosis is a multi-system disease of unknown
etiology, usually affecting the respiratory tract and other organs, and is
characterized by the formation of nonnecrotizing epithelioid granulomas. The
diagnosis depends on a combination of a typical clinicoradiological
presentation, the finding of nonnecrotizing epithelioid granulomas in a tissue
biopsy, and exclusion of other possible diseases, especially those of
infectious etiology.
Sarcoidosis results from an uncontrolled
cell-mediated immune reaction. Interactions between chemokines and receptors
that activate mitogen-activated protein kinase pathways play a major role in
inflammation and T-cell responses. Tumor necrosis factor (TNF)-[alpha] is an
important player in granuloma formation, and recent clinical trials have
investigated the efficacy of TNF-[alpha] inhibitors in sarcoidosis.
HRCT view of cannonball secondaries
Ever wondered how cannon ball secondaries are seen on HRCT thorax??? Go through the video to find the cannon ball secondaries on HRCT thorax..
Unable to view the video watch it in youtube
Want to Know more about cannon ball secondaries? Read this article
The HRCT findings of Bronchiectasis.
Pulmonary Medicine Blog By Dr Deepu
Does this look like a gloved finger???
CT findings in bronchiectasis include the
following:
· Let me first describe the specific findings in the bronchiectasis
Has parallel tram track lines, or
It may have a signet-ring appearance,
Let me make it more clearer, it is composed of a dilated bronchus cut in a horizontal section representing the golden ring; with an adjacent pulmonary artery representing the stone of the Ring. Take a look at the signet ring to get the idea.
· The diameter of the bronchus lumen is normally 1-1.5 times that of the adjacent vessel; a diameter greater than 1.5 times that of the adjacent vessel suggests bronchiectasis. Let us correlate it in the CT scan
Second Sign is lack of bronchial tapering, Normally as we move to the peripheral parts of the HRCT, the Bronchus should start tapering, as the diameter of the bronchus progressively decreases, whereas in the patients with bronchiectasis this tapering is not seen as the bronchial wall is destroyed and dilated , see the images below
 |
| NORMAL BRONCHIAL TAPERING |
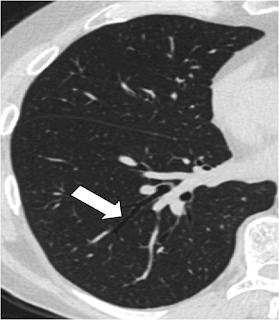 |
| LACK OF BRONCHIAL TAPERING |
We can also see the abnormal bronchial contour due to the tractional forces applied by the fibrosed and diseased lungs
Visibility of peripheral airways within 1 cm of the pleura
Normally airways are not seen upto 1 cm from the pleura but with bronchiectasis we may be able to see the dilated peripheral airways
 |
| ARROWS POINTING TO THE DILATED PERIPHERAL AIRWAYS WITHIN 1 CM OF PLEURA |
Its time to describe the non specific findings in the bronchiectasis
•Peribronchial cuffing (thickened hazy bronchial wall).
•Finger in glove opacities
(mucus filled bronchi).
•Multiple air fluid levels
(fluid filled bronchi).
Peripheral cuffing- here we have a thickened bronchial wall due to constant underlying inflammatory process in the bronchial wall
 |
| PATIENT WITH LONG STANDING ABPA SHOWING BRONCHIECTASIS IN THE RIGHT LUNG, WITH BRONCHIAL WALL THICKENING |
Finger in glove opacities( Mucus filled bronchi)
mucus plugging of the bronchus causes bronchus to appear as a gloved hand
let us see how it appears in the CT Scan
Next sign is multiple air fluid levels
Along with these specific and non specific finding we will be able to see few ancillary findings associated with bronchiectasis
•Mosaic perfusion.
•Air trapping.
•Tree in bud opacities.
Mosaic Perfusion
Air Trapping, to see air trapping specifically ask for expiratory film, the air gets trapped in the blocked small airways causing dark areas, whereas the air is squeezed out from normal lung.
Tree in Bud Appearance-
occurs due to active infection, study the image and find tree in bud, I have marked it in 2nd image
occurs due to active infection, study the image and find tree in bud, I have marked it in 2nd image
 |
| Image shows bronchiectasis and tree in Bud |
tIf you liked the post please comment , comments activates the search engine, Thanks
Suggested Reading
The Rings !!!The Trams!!!, Chest X Ray Findings in Bronchiectasis
My Next post will be on "SOLITARY PULMONARY NODULE"
The ‘Dark Bronchus’ Sign: For diagnosis of PCP
Pulmonary Medicine Blog By Dr Deepu
Today I will discuss the importance of the ‘dark bronchus’ sign in
the diagnosis of uniform, diffuse ground glass opacification on high resolution
computerized tomography (HRCT). This sign is useful to identify diffuse ground
glass opacity on HRCT in cases of Pneumocystis carinii pneumonia who may
present with a normal or equivocal chest radiograph in the early course of
disease.
Chest radiograph is the initial investigation in HIV patients with
chest symptoms. But even in patients with proven PCP, radiographic findings may
be normal in up to 20-40%. Low incidence of PCP in patients with normal or
equivocal findings on chest radiograph despite high clinical suspicion
emphasizes the need for a noninvasive and widely available investigation in
such cases.
Various modalities to investigate symptomatic HIV patients with
normal, equivocal or nonspecific radiographic findings include carbon monoxide
diffusion in lung (DLCO), gallium citrate lung scanning and HRCT. A DLCO of
less than 80% of the predicted value has a sensitivity of up to 98% for PCP,
but the specificity is less than 50% and the measurement is not always
available. Although gallium scanning has a sensitivity of up to 100% for PCP in
patients with abnormal radiographs, it has never been prospectively studied in
patients with normal or equivocal radiographic findings. In addition, this
investigation requires a 48- to 72-hour delay in imaging, is not readily
available and has a high cost.
On the other hand, HRCT
is a widely available and noninvasive investigation for PCP. Patchy or diffuse
ground glass opacity is the most frequent finding. Other findings include
cystic changes (33%), centrilobular nodules (25%), lymphadenopathy (25%) and
pleural effusion (17%). HRCT has been found to be especially important in the
assessment of symptomatic patients with normal, equivocal or nonspecific
radiographs. In such cases, it shows high sensitivity (100%), specificity (86%)
and accuracy (90%) for PCP, using only the presence or absence of ground glass
opacity as the criterion for positivity.
 |
| The Arrow Shows The Dark Bronchus Relative to The Surrounding Lungs |
Patchy ground opacity or mosaic attenuation, which is observed in up to 92% of the patients, can be easily identified on HRCT. However, subtle ground glass opacification, especially when bilateral and diffuse, may be difficult to diagnose. This is because of bilateral uniform increase in lung attenuation with absence of normal lung parenchyma for comparison. In such cases, the ‘dark bronchus’ appearance is a useful sign to identify diffuse ground glass opacity. This finding refers to the presence of air-filled bronchi appearing ‘too black’ relative to the surrounding lung parenchyma, which is filled with inflammatory alveolar exudates. This subtle finding may help in identification of patients with ‘possible PCP’ despite a normal or equivocal chest radiograph. Subsequently direct test for PCP (i.e., broncho-alveolar lavage) may be initiated for definitive diagnosis and treatment.
Hence the importance of the ‘dark bronchus’ sign in the diagnosis of uniform, diffuse ground glass opacification on HRCT. This is especially useful in the presence of a normal chest radiograph and ‘near normal’ HRCT. HRCT offers an accurate and early diagnosis in patients with normal chest radiographs; it alters patient management and facilitates early therapy.
Also Read
Hence the importance of the ‘dark bronchus’ sign in the diagnosis of uniform, diffuse ground glass opacification on HRCT. This is especially useful in the presence of a normal chest radiograph and ‘near normal’ HRCT. HRCT offers an accurate and early diagnosis in patients with normal chest radiographs; it alters patient management and facilitates early therapy.
Also Read
BASICS OF HRCT PART 7 - DIFFERENTIAL DIAGNOSIS OF ILD
This is the last post in the series of basics of HRCT. links to the previous posts are given at the end of this post.
DIFFERENTIAL DIAGNOSIS OF INTERSTITIAL LUNG DISEASE
DIFFERENTIAL DIAGNOSIS OF INTERSTITIAL LUNG DISEASE
Reticular pattern
1.
Lymphangitic
carcinomatosis: irregular septal thickening, usually focal or unilateral 50%
adenopathy', known carcinoma.
2.
Cardiogenic pulmonary
edema: incidental finding in HRCT, smooth septal thickening with basal
predominance (Kerley B lines), ground-glass opacity with a gravitational and
perihilar distribution, thickening of the peribronchovascular interstitium
(peribronchial cuffing)
3.
Lymphangitic
carcinomatosis.
4.
Lymphangitic
carcinomatosis with hilar adenopathy.
5.
Alveolar proteinosis:
ground glass attenuation with septal thickening (crazy paving).
6.
Cardiogenic pulmonary
edema.
Nodular pattern
1.
Hypersensitivity
pneumonitis: ill defined centrilobular nodules.
2.
Miliary TB: random
nodules
3.
Sarcoidosis: nodules
with perilymphatic distribution, along fissures, adenopathy.
4.
Hypersensitivity
pneumonitis: centrilobular nodules, notice sparing of the area next to pleura
and fissure.
1.
Sarcoidosis: nodules
with perilymphatic distribution, along fissures, adenopathy.
2.
TB: Tree-in-bud
appearance in a patient with active TB.
3.
Langerhans cell
histiocytosis: early nodular stage before the typical cysts appear.
4.
Respiratory
bronchiolitis in infection.
1.
Chronic eosinophilic
pneumonia with peripheral areas of ground glass opacity.
2.
Sarcoid end-stage with
massive fibrosis in upper lobes presenting as areas of consolidation. Notice
lymphadenopathy.
3.
Chronic eosinophilic
pneumonia with peripheral areas of consolidation.
4.
Broncho-alveolar cell
carcinoma with both areas of ground glass opacity and consolidation
1.
Non specific
interstitial pneumonitis (NSIP): ground glass with traction bronchiectasis, no
honeycombing.
2.
Cryptogenic organizing
pneumonia (COP).
3.
Sarcoidosis end-stage:
consolidation as a result of massive fibrosis perihilar and in upper lobes.
4.
COP.
1.
Lymphangiomyomatosis
(LAM): uniform cysts in woman of child-bearing age; no history of smoking;
adenopathy and pleural effusion; sometimes pneumothorax.
2.
LCH: multiple round
and bizarre shaped cysts; smoking history.
3.
Honeycombing
4.
Centrilobular emphysema:
low attenuation areas without walls.
1.
Centrilobular
emphysema: low attenuation areas without walls. Notice the centrilobular artery
in the center.
2.
Langerhans cell
histiocytosis (LCH): multiple thick walled cysts; smoking history.
3.
Honeycombing.
4.
Lymphangiomyomatosis
(LAM): regular cysts in woman of child-bearing age.
suggested reading
BASICS OF HRCT PART 6 - DISTRIBUTION PATTERN AND ADDITIONAL FEATURES
Upper lung zone
preference is seen in:
- Inhaled particles: pneumoconiosis (silica or coal)
- Smoking related diseases (centrilobular emphysema
- Respiratory bronchiolitis (RB-ILD)
- Langerhans cell histiocytosis
- Hypersensitivity pneumonitis
- Sarcoidosis
Lower zone preference is seen in:
- UIP
- Aspiration
- Pulmonary edema
Peripheral
distribution is mainly
seen in cryptogenic organizing pneumonia (COP), chronic eosinophilic pneumonia
and UIP.
Additional findings
Pleural effusion is seen in:
1.
Pulmonary edema
2.
Lymphangitic spread of
carcinoma - often unilateral
3.
Tuberculosis
4.
Lymphangiomyomatosis
(LAM)
5.
Asbestosis
Hilar and mediastinal lymphadenopathy
In sarcoidosis the common pattern is right paratracheal and bilateral hilar adenopathy ('1-2-3-sign').
In lung carcinoma and lymphangitic carcinomatosis adenopathy is usually unilateral.
'Eggshell calcification' in lymph nodes commonly occurs in patients with silicosis and coal-worker's pneumoconiosis and is sometimes seen in sarcoidosis, postirradiation Hodgkin disease, blastomycosis and scleroderma .
read other posts in this series
Subscribe to:
Comments (Atom)






















.jpg)
.jpg)
.jpg)



.jpg)
.png)
.png)

.png)